Do all cavernous malformations bleed?
Hemorrhage risk depends on the stage of a cavernous malformation (cavernous angioma, cavernoma) lesion. Cavernous malformations are categorized into two groups, called Stage 1 and Stage 2 lesions.
A Stage 1 lesion is in the earliest stages of development. Typically, it is a single dilated cavern and only visualized at the highest field MRI technologies because they are only 1-2 mm in size. Stage 1 lesions have not bled outside of the lesion.
A Stage 2 lesion is a multi-cavernous lesion with multiple dilated blood vessels. They are mulberry-shaped, often prone to hemorrhage, and readily seen on MRI. On the T2 weighted sequence of an MRI, they have a popcorn appearance.
Stage 2 lesions are larger than 3 mm (0.1 inches) and can grow much larger, 2.5 cm (1 inch) or more. We know a Stage 2 cavernous malformation has bled because it is surrounded by a hemosiderin ring which is easily seen on MRI. Hemosiderin is a blood breakdown product, and its presence indicates that blood has leaked outside of the cavernous malformation. The blood may have oozed slowly out of the lesion over time or may have hemorrhaged a larger amount of blood over the course of days.
Do all hemorrhages cause symptoms?
No, it is possible to have a small asymptomatic hemorrhage depending on the location of the lesion. Research indicates these hemorrhages occur more often in lesions that will go on to have a symptomatic hemorrhage. Hemorrhage activity can be seen on MRI even in the absence of symptoms.
If I have a symptomatic hemorrhage, what symptoms can I expect?
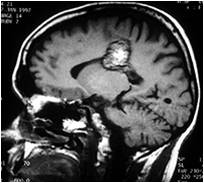
Those who have brainstem lesion hemorrhages can experience multiple and diverse symptoms (focal neurological deficits) possibly including double vision, facial droop, balance problems, and difficulty swallowing.
It is important to talk with your doctor about what symptoms you could expect given the location of your lesion.
On rare occasions, patients have hemorrhages large enough to cause “mass effect,” meaning that brain tissue is shifted to make room for the lesion. This can result in increased intracranial pressure or, possibly, hydrocephalus. In an infant, this may be the first sign that a hemorrhage has occurred. Increased intracranial pressure can result in pupil and vision changes, nausea, projectile vomiting, headache, confusion, and impaired consciousness
What is my risk of having a first hemorrhage or a subsequent hemorrhage?
According to the cavernous malformation Clinical Care Guidelines, it is estimated that the rate of having a symptomatic first hemorrhage is about 0.4%-2.4% per year. Following an initial symptomatic hemorrhage, the rate of rebleed can range from 3.8%-29.5% per year. Patients with lesions located in the brainstem are at a higher risk for symptomatic hemorrhage. Finally, we know through several studies that lesions that have hemorrhaged are most likely to re-hemorrhage within five years of their first bleed (estimated 42% risk). After this, re-hemorrhage rates drop substantially.
If your cavernous malformation was discovered “incidentally”, that is, you had an MRI for a different issue and the cavernous malformation was spotted but was asymptomatic, your chance of hemorrhage is very, very low (0.08% per patient-year). A 2014 study out of Mayo Clinic tracked 107 patients with incidental lesions for a total of 1311 patient-years over more than 10 calendar years. Only two hemorrhages were recorded in the group over this period.
A 2015 Mayo study determined that among their patients, hemorrhage was more likely during fall and winter than during spring and summer, possibly because of lower Vitamin D levels or increased exposure to flu.

Will I need to have surgery if I’ve had a hemorrhage?
In general, surgery is not recommended if you are asymptomatic, especially if the cavernous malformation is located in a deep or infratentorial location, such as the brainstem.
If you have had a symptomatic hemorrhage in a location that is considered to be easily accessible, then surgery may be recommended. Surgery becomes more challenging in deeper or more eloquent locations, such as the brainstem, but may also be considered if you have had a previous hemorrhage and if the risk of not having surgery outweighs the natural history course of the disease for that location.
Ultimately, choosing to have surgery is an individual decision and it is best to weigh the risks and benefits with your surgeon. While recovery from a hemorrhagic event normally occurs, surgery can come with the risk of developing new symptoms or worsening status.
If you have had a symptomatic hemorrhage and surgery is not indicated, a follow-up MRI within three months is recommended. We also ask that you read more about participating in a clinical drug trial of medicines being tested to reduce the risk of re-hemorrhage.
Am I at a greater risk of hemorrhage during pregnancy?

The vast majority of women complete a pregnancy without hemorrhage or need for surgical removal of an angioma. Unless you have had a recent hemorrhage or other neurological deficit preventing a vaginal delivery, there are no contraindications for having a vaginal birth.
Pregnancy is a time of intense physiologic changes for mother and baby, and the consequences of hemorrhage or seizure may be more complicated than in the non-pregnant state. Any patients with neurovascular problems and/or epilepsy are urged to have their pregnancy overseen by a high-risk obstetrician. Your obstetrician should work in close coordination with a neurologist or neurosurgeon that is familiar with your neurological history and who is knowledgeable about cavernous malformations and about epilepsy in pregnancy.
If symptoms, such as seizure or severe acute headache, develop during pregnancy, an MRI without contrast is recommended. If a hemorrhage occurs, the risks and benefits of having surgery should be examined on an individual basis.
Will taking a blood thinner increase my risk of hemorrhage?
In general, blood thinners have not been recommended for people with cavernous malformation due to the potential risk of bleeding. A 2019 study published in The Lancet concluded that if you need to take an anti-thrombotic for another medical condition and your CCM disease has been stable for a year or more, particularly if you have the sporadic form of the illness, you should feel reassured that you can do so safely. In this case, Dr. Kelly Flemming, co-author and a member of the Alliance to Cure Cavernous Malformation Scientific Advisory Board, urges consultation with a doctor well-versed in CCM who can verify that your illness is stable, and she also urges keeping the course of blood thinners short, if possible. An in-depth discussion of this topic can be found in a Blood Thinners and CCM webinar we hosted in early 2020.
It is safe to take acetaminophen (paracetamol). This medicine does not influence bleeding tendency.
In a 2022 Mayo study, researchers found that fish oil and SSRI medicines do not appear to increase the risk of hemorrhage.
To learn more, please visit our page on blood thinners.
Is there anything I can do to prevent a future hemorrhage?
Inflammation has been implicated in cavernous malformation hemorrhage. Here are recommendations from the Scientific Advisory Board to control systemic inflammation:
- Maintain normal vitamin D levels and supplement accordingly under your doctor’s supervision
- Quit smoking
- Receive an annual flu vaccine and recommended COVID vaccines
- Treat sleep apnea
- Maintain a preservative-free diet
- Treat high blood pressure.
- Stay stress-free. Of course, this is much easier said than done! Dr. Issam Awad, Chair of the Alliance to Cure Cavernous Malformation Scientific Advisory Board, notes that stress can alter neurological symptoms after a stroke and can account for fluctuations of symptoms. There is no known physiologic or hormonal basis for this. However, stress can increase blood pressure, which could be a problem in hypertensive patients with increased hemorrhage risk.
Visit our Lifestyle Management section for more information and to learn how you can best support your health while living with cavernous malformation.
Patients with CCMs can:
- Engage in aerobic activity and noncontact sports. A 2020 study completed at Mayo reported that these activities have not been shown to increase hemorrhage risk. Less is known about contact sports, high-altitude climbing, scuba diving, and those with spinal-cord cavernous malformation.
- Give birth vaginally as long as the CCM is closely managed during the term of pregnancy.
- Fly in commercial aircraft with normal cabin pressures.
- Consume alcohol and caffeinated beverages in moderation.
Researchers are examining the risk of hemorrhage related to the use of hormonal agents, Botox use, and probiotics.
Dr. Issam Awad notes that there has been some relation shown between diet pills, certain stimulants, and nasal decongestants containing phenylpropanolamine and intracranial hemorrhage in young patients, including, possibly, in cases with CCM. These items have been taken off the shelves by the FDA, but it is possible that other excessive stimulants might cause bleeds.
He explains that stimulants may increase blood pressure in hypertensive patients, and this could contribute to a predisposition to hemorrhagic stroke. Extreme stimulants such as cocaine and other illicit drugs have been shown to cause brain hemorrhages among patients without prior history of high blood pressure, including cases with pre-existing vascular malformations.
Summary
Because questions remain regarding the natural history of CCMs, the mechanism by which these lesions hemorrhage and the resultant consequences are not fully understood. The important consideration is that patients can lead long and healthy lives even after a hemorrhagic event. Maintaining low inflammation in the body by leading a healthy lifestyle, monitoring vitamin D levels, and minimizing stress, are all great ways to lower your risk of hemorrhage.
Should symptoms suddenly appear, don’t delay in getting an MRI and consulting with a neurosurgeon that has extensive experience managing and treating CCMs. In this case, ignorance is not bliss!
Updated 4.16.2022
References
- Previch L et al. The Influence of Select Medications on Prospective Hemorrhage Risk in Patients with Spinal or Cerebral Cavernous Malformations. World Neurosurg. 2022 Mar 29;S1878-8750(22)00395-3. doi: 10.1016/j.wneu.2022.03.101Carrión-Penagos J, Zeineddine HA, Polster SP, Girard R, Lyne SB, Koskimäki J, Romanos S, Srinath A, Zhang D, Cao Y, Stadnik A, Piedad K, Shenkar R, Awad IA. Subclinical imaging changes in cerebral cavernous malformations during prospective surveillance. J Neurosurg. 2020 Apr 3;1-8.
- Flemming KD, Kumar S, Brown RD Jr, Lanzino G. Predictors of initial presentation with hemorrhage in patients with cavernous malformations. World Neurosurg. 2020 Jan;133:e767-e773.
- Flemming K, D, Kumar S, Brown Jr R, D, Singh R, J, Whitehead K, McCreath L, Lanzino G. Cavernous malformation hemorrhagic presentation at diagnosis associated with low 25-Hydroxy-Vitamin D level. Cerebrovasc Dis. 2020;49:216-222. doi: 10.1159/000507789.
- Joseph NK, Kumar S, Lanzino G, Flemming KD. The Influence of Physical Activity on Cavernous Malformation Hemorrhage. J Stroke Cerebrovasc Dis. 2020;29(4):104629. doi:10.1016/j.jstrokecerebrovasdis.2019.104629
- Joseph NK, Kumar S, Brown Jr RD, Lanzino,G, Flemming KD. Influence of pregnancy on hemorrhage risk in women with cerebral and spinal cavernous malformations. Stroke. 2021 Jan;52(2):434-441. doi: 10.1161/STROKEAHA.120.031761.
- Zuurbier, Susanna M et al. Long-term antithrombotic therapy and risk of intracranial haemorrhage from cerebral cavernous malformations: a population-based cohort study, systematic review, and meta-analysis. The Lancet Neurology. 2019;18(10):935-941.
- Awad IA, Polster SP. cavernous malformations: deconstructing a neurosurgical disease. J Neurosurg. 2019;131(1):1–13.
- Akers A, et al. Synopsis of guidelines for the clinical management of cerebral cavernous malformations: consensus recommendations based on systematic literature review by the Alliance to Cure Cavernous Malformation Scientific Advisory Board Clinical Experts Panel. Neurosurgery. 2017;80(5):665–680.
- Girard, R., Khanna, O., Shenkar, R., Zhang, L., Wu, M., Jesselson, M., Zeineddine, H. A., Gangal, A., Fam, M. D., Gibson, C. C., Whitehead, K. J., Li, D. Y., Liao, J. K., Shi, C., & Awad, I. A. (2016). Peripheral plasma vitamin D and non-HDL cholesterol reflect the severity of cerebral cavernous malformation disease. Biomarkers in Medicine, 10(3), 255–264. https://doi.org/10.2217/bmm.15.118
- Horne MA, Flemming KD, Su IC et al. Clinical course of untreated cerebral cavernous malformations: a meta-analysis of individual patient data. Lancet Neurol. 2016;15(2):166–173.
- Moore SA, Brown RD Jr, Christianson TJ, Flemming KD. Long-term natural history of incidentally discovered cavernous malformations in a single-center cohort. J Neurosurg. 2014;120(5):1188–1192.
- McDonald DA, Shenkar R, Shi C, Stockton RA, Akers AL, Kucherlapati MH, Kucherlapati R, Brainer J, Ginsberg MH, Awad IA, Marchuk DA. A novel mouse model of cerebral cavernous malformations based on the two-hit mutation hypothesis recapitulates the human disease. Human Molecular Genetics, Volume 20, Issue 2, 15 January 2011, Pages 211–222.


